Dental Supplies Blog

July 21 2025
What is the Best Dental Cement for Crowns and Bridges
What’s the Best Dental Cement for Crowns and Bridges
July 18 2025
Textured vs. Smooth Nitrile Gloves
Textured vs. Smooth Gloves: What Orthodontists Should Know

February 12 2025
Ultrasonic scalers
Power scaling devices are either ‘sonic’, vibrating between 3,000 and 8,000 times per second, or ‘ultrasonic’, operating between 20,000 and 50,000 Hz. The ultrasonic ones tend to work better than the sonic kind, deplaquing and flushing the periodontal pocket well, and destroying bacterial cell walls with cavitating bubbles in their water streams. Ultrasonic scalers are either ‘magnetostrictive’, where energy is converted to elliptical strokes in the unit's metal rod, or ‘piezoelectric’, where strokes go in a linear pattern, back and forth, regulated by crystals in the ceramic handpiece.

February 10 2025
Bands or crowns in space-maintaining orthodontia?
We’ve written before about choosing your orthodontic supplies. We said the key considerations are brand reputation, functional utility, durability, and quality of after-sale support.
Let’s do a little deep-dive.
One of the orthodontic things we supply is kits full of space-maintainer bands, for kids who lose molars early. As you know, the idea is to keep gaps open for the eruption of new molars. During this time, the concern is for good hygiene around those bands, for healthy gingiva.

October 17 2024
High Definition Black Line Mirrors
Designed for enhanced performance, our HD Black Line Mirror is engineered to optimize clinical outcomes by delivering superior visibility throughout any dental procedure. The Diamond Like Carbon (DLC) coating of the handle and mirror frame reduces glare up to 80%!* The durable black matte finish in combination with the superior brilliance and color of our proprietary HD Mirror glass facilitates quicker and more accurate visibility of the mouth.

November 19 2020
How Gingival Retraction Drives Restorative Excellence
Producing an exceptional restoration for a damaged tooth involves a series of complex, inter-related steps. When a set of restorations are completed together, such as for a smile makeover or full mouth rehabilitation, each step’s importance increases. One mismanaged piece can turn a masterpiece into a disaster. From planning to the final polish, the delivery of excellence rests on crucial principles.

September 27 2020
3 Must-Have Tools For Successful Endodontics
Dentists face a challenging question every day: Should a damaged natural tooth be maintained with endodontic and restorative treatment, or should it be replaced with an implant? Implants continue to grow in popularity, and over five million implants are placed in the U.S. every year. But many times, endodontic therapy helps preserve a tooth and eliminates more invasive treatment.
More than 15 million root canals are completed annually in the U.S., and general dentists do nearly 11 million of them. Five million dental implants will be placed, too. Each situation requires a series of decisions to determine the best option.
July 26 2020
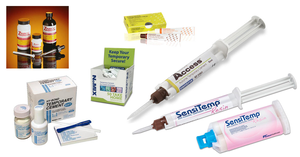
Temporary Dental Cement Solutions: Six Unique Products That Save Time, Money, and Space
Dental cement products provide a critical tool for dentists to deliver exceptional clinical care. When fabricating a custom lab-based restoration, dentists need a reliable temporary cement during the interim period. But when the final restoration comes back from the lab, a temporary restoration must be easy to remove. And the new restoration needs adhesion that gives both the clinician and patient confidence for years of service.

June 28 2020
5 Keys To Aerosol Reduction in Dental Settings
In dentistry, many procedures using high-speed handpieces and ultrasonic instruments produce aerosols, small droplets that suspend in the air. Viral particles, bacteria, and fungi can travel through aerosols, similar to what happens when someone sneezes. In some cases, these particles can go up to 20 feet and stay suspended in the air for several hours.
Dental staff who perform procedures on patients find themselves at risk or exposure to many pathogens. The highest risk develops from splatter to the face of clinicians and to the nasal region of patients. Periodontal procedures using ultrasonic and sonic instruments transmit the greatest number of droplets. Air polishing, use of the air/water syringe, and the operation of a high-speed handpiece also produce aerosols.

June 17 2020
AMALGAM ALLOYS
A large number of dental restorative materials having different properties have been available in the market. Specialist dental professionals choose the required restorative materials according to the variable requirements intended in each patient. Dental amalgam alloys have been considered as the most commonly used restorative option since ages with the utmost durability and ease of manipulation. This alloy is a popular restorative biomaterial containing mercury in a liquid form in metal alloy forming a mixture. At skydentalsupply, Silver, tin, copper and traces of certain other metals in liquid mercury produce a mixture with great strength, durability, resistance to fracture and longevity which is much needed for restoring the molars involved in everyday chewing and mastication of food.

May 20 2020
What’s new in infection control?
There’s been a busy round of papers recently, about pathogens and contagions in dental practices. It’s easy to guess why. They all kind of say what all of us pretty much expect, but it is nice to see people looking at the problem again, and totting up more stats about it. Numbers are always good. Even more fortuitously, there are good review articles out there, or in process, so it’s easy to scope out current thinking. As always, we’ve done this, with our busy customers in mind.

March 15 2020
Should you buy toys for your pediatric dental patients? A large new study says yes.
‘Dental Accessories’ means a lot of things. In our catalogue it refers to gizmos that make your office all ergonomic, or trays and tubs that keep you organized, or patient education tools – novelty items, really, that patients like to have, so you can keep them engaged and coming back. Or it means toys, dental-themed, for the youngsters in your chair.
Personalities vary. Some clinicians are pretty impatient with the whole concept of toys in the office. Others, possibly the ones with little kids of their own, think it’s a good idea. They put things to play with out in the waiting area, and sometimes let them come right into the operating room with their little patients.
January 27 2020
What’s the latest word on bone substitutes for implant therapy?
We talk with our customers all the time. We like to keep track of what’s on their minds professionally, and we like to keep them up-to-date on industry trends.
Lately there’s been a lot of discussion about guided bone regeneration, for alveolar ridge augmentation. The idea is to build up stable space for infiltration of osteogenic cells, and get angiogenesis underway as quickly as possible.
January 14 2020
Pit and fissure sealant versus fluoride varnish – which really is better prevention?
Talking to our customers over the years, and keeping track of what they buy, has taught us that strategies for clinical intervention are sometimes a matter of simple preference, not scientific data. That happens because the data as to which route to choose simply isn’t there.
This is very much the case in the matter of caries prevention. The two basic strategies are pit and fissure sealing and fluoride varnishing. They both work, and they’re both in wide use – but the relative effectiveness of the two is not at all clear, even after all their years in use.
December 19 2019
What’s the best root canal sealer for biocompatibility?
If you do root canals, you’ll use the kind of sealer you were trained to use, or the kind you’re used to using, or the kind that seems to work best for you. We’re largely creatures of habit.
But sealers aren’t all the same.
Ideally, every sealer should be easy to mix, and should adhese nicely, and should seal well, with no shrinking or staining. It shouldn’t dissolve over time, but it should be soluble enough that you can take it out easily if you need to. it should be bacteriostatic, and it should show up clearly in radiography. Above all, it should be as biocompatible as possible, so it doesn’t irritate periradicular tissue.
